TRUE SPINAL DECOMPRESSION THERAPY fOR HERNIATED DISC
Spinal Decompression is a non-surgical and drug-free answer for disc related syndromes of the lumbar and cervical spines when chiropractic, physical therapy and traditional allopathic treatments fail. Many people have found relief from pain associated with herniated discs, bulging discs, degenerative joint disease, and other spinal disorders.
Spinal decompression uses computer aided technology to apply gentle, decompression to your spine. There is a big difference between traction, distraction and decompression therapy. Spinal Decompression therapy at Golden Acupuncture & Chiropractic in Fairfax, VA is a unique combination of restraint, treatment parameters, angle position and equipment engineering.
True spinal biomechanics and the ability to use them can make the difference between a patient getting well, and being destined to a life of pain and misery. After thorough evaluation, your decompression specialist will customize proper spinal decompression protocols to correct the problem.
These protocols include, proper patient placement, absolute and exact spinal positioning for maximum lesion reduction, and knowing the proper setup for the decompression unit and the right treatment parameters.
Each treatment session averages 15 to 30 minutes in duration. On average, herniated discs generally respond within 5 – 20 sessions. Spinal decompression therapy is often very successful to treat sciatica or radiating pain by correcting herniated disc or spinal disorder.
Call our office to schedule your consultation and learn if you are a candidate for Spinal Decompression Therapy.
Type of Disc Diseases
The disc can be damaged through a major trauma like lifting heavy object or by repetitive micro-trauma over a period of time. The result of these traumas can be that the disc will thin out, degenerate, bulge, or herniate.
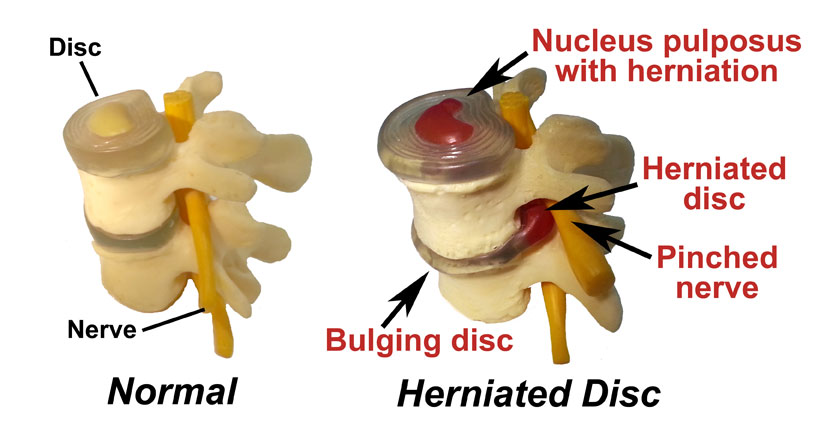
The cartilage of the outer walls of the disc are damaged or weakened to varying degrees due to trauma. As pressure is put onto a disc, the inner material of the disc (nucleus pulposis) is pushed outward. The cartilage wall that is trying to hold in this inner “jelly” material has been weakened.
- Disc Degeneration or Spinal Stenosis – This is aging related condition of the discs between vertebrae with loss of cushioning, fragmentation and herniation. Disc degeneration has less space for spinal nerves to exit from the spinal cord, causing pinched nerve symptoms.
- Bulging Disc – Push out the cartilaginous wall of the disc causing a bulging disc. It is like a bubble in a tire. This bulging disc can put pressure against the spinal cord or nerve being “pinched”.
- Herniated Disc – This is a condition when some of the soft “jelly” pushes out through a tear in tougher exterior. This herniated disc can compress nerves and cause sharp pain, numbness or weakness in an arm or leg.






